The News and Observer (our local paper here in the Triangle) recently ran a great story on overuse injuries in young athletes. I firmly believe this is one of the fastest growing injuries I see in the clinic and in many cases it is preventable. One of the biggest issues now is this commonplace idea that gifted athletes should play the same sport year-round to get ahead.
I remember growing up as a kid and playing football, basketball and baseball in the fall, winter and spring. While AAU basketball and Legion ball existed, most kids were still playing multiple sports. Over my 15 years as a physical therapist I have witnessed several of these one sport stars see their playing time and bodies take a hit due to injury.
The American Orthopedic Society for Sports Medicine (AOSSM) and the American Academy of Orthopedic Surgeons (AAOS) state that overuse injuries account for nearly half of the 2 million injuries seen among high school athletes each year. While soccer and swimming seem to send many athletes into PT, any repetitive throwing or overhead activity bears considerable risk for an eventual shoulder or elbow problem as well. Some of the common injuries I typically see are:
- Patellofemoral pain
- Shin splints
- Rotator cuff injury
- Bursitis
- Shoulder instability
- Little League elbow
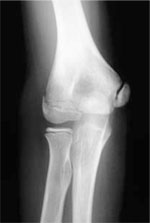
Little League Elbow (medial epicondylar apophysitis)
These injuries are just some of the most common ones I see. In the article, the reporter focused on baseball and throwing. With that in mind, consider research published in the American Journal of Sports Medicine this past February from renowned surgeon James Andrews that revealed players who pitch more than 100 innings in a calendar year are 3.5 times more likely to be injured.
He goes on to say that “these injuries are the result of a system that prepares genetically gifted athletes to play at the highest levels, but eliminates most players because their bodies cannot withstand such intense activity at such an early age.” Sadly, he told the reporter that in 1998 he performed the Tommy John procedure on 5 kids high school age or younger, while in 2008 he did the same procedure on 28 children in the same age range. This injury is usually caused by throwing too much too soon.
Consider the following data on suggested pitch counts per game (source James Andrews, MD & Glenn Fleisig, MD):
- 8-10 y/o = 52 plus/minus 15 pitches
- 11-12 y/o = 68 plus/minus 18
- 13-14 y/o = 76 plus/minus 16
- 15-16 y/o = 91 plus/minus 16
- 17-18 y/o = 106 plus/minus 16
Unfortunately, I can personally relate to this blog post and story. I was a promising young pitcher up until the point I threw my arm out in travel baseball at age 13. The pain got so bad in my arm I could barely throw a ball 10 feet. I remember the orthopedic surgeon telling me that I could not throw again the rest of the summer. The pain (and memory of it) was so bad I elected to focus on position play and not to pitch again until my senior year of high school. At that point, my arm was no longer the same as I had missed three years of practice and development. Now, I too had become one of those kids whose body was never the same.
So, as a rehab and strength & conditioning professional, I want to help educate and promote better awareness to athletes, parents, coaches, trainers, AD’s, ATC’s and anyone who is involved in the care and training of young athletes. Fortunately, people are taking positive steps to reduce overuse injuries. One great initiative is STOP – Sports Trauma Overuse Prevention and you can learn more by clicking here to visit their website.
In the end, we must continue to educate everyone that the old motto of “No Pain, No Gain” is NOT the way to handle overuse injuries as this mentality may ruin the careers of young athletes or lead to an otherwise preventable injury and/or premature musculo-skeletal damage. Pain truly is a warning signal the body gives us to detect mechanical problems and make changes in our training/activity level until we sort out the cause and solution. I hope you will join me in supporting this mission and working hard at making sports fun, safe and free of overuse injuries for young athletes of all ages in the years to come.
References – The News & Observer – May 15, 2011





